C-section Birth & the Microbiome
Giving birth is one of the most profound experiences of life, occurring every second of every day all over the world. It can also be one of the most overwhelming experiences, especially when pregnancy complications arise.
According to the World Health Organization, cesarean section (C-section) use continues to rise globally. As a result, we’re seeing more research focusing on the health of these babies, with a specific focus on the microbiome differences between C-section and vaginal delivery.
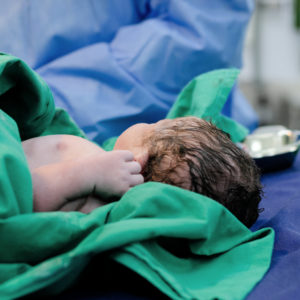
What’s a C-section birth?
There are a variety of delivery methods for giving birth. The two main categories are vaginal delivery and cesarean section. Vaginal delivery is the most common type of birth where the baby comes out through the birth canal. A cesarean section delivery is a surgical procedure for delivering one or more babies through incisions in the mother’s abdomen and uterus.

Where does the term “cesarean” originate from?
The answer to this question is surprisingly unclear, despite being thoroughly investigated. There are tales that cesarean originated from the birth of Roman leader Julius Caesar back in 100 BC, but most historians disagree. The most accepted origin theory believes cesarean stems from the Latin word caedere, which means to cut.
According to data collected by the National Center for Health Statistics, about 1 in 3 babies in the United States are born via C-section. Although C-sections can be scheduled for many specific reasons, the need for a first-time C-section birth is often not known until labor has started. A doctor may recommend a C-section for the following reasons: labor not progressing, baby in distress, baby measuring large or in an abnormal position, mother carrying multiple babies, problems with placenta, prolapsed umbilical cord, and mechanical obstruction.
Birth After C-section
A common question women have after undergoing a C-section is whether or not they can give birth again. Thankfully, the answer is yes! But it is imperative to allow the body time to heal and recover from the procedure. The suggested time to wait before conceiving again varies from 6 to 24 months, depending on multiple factors. However, most experts advise waiting at least 12 to 15 months before trying to conceive again.
Depending on the medical reason for having a C-section birth the first time, a mother may be advised to have an elective repeat C-section (ERCS) for her next birth. Vaginal birth after a C-section (VBAC) is also an option. Either method for delivery after a C-section should be researched thoroughly with a medical provider to see what is the safest option for the mother and baby.

C-sections are essential and save lives.
Unfortunately, C-sections can also put mothers and their babies at unnecessary health risks when performed for no medical need. Sometimes, requests for a first-time birth via C-section occur for the convenience of a planned delivery or for the avoidance of labor and possible complications of vaginal birth. Although these reasons may seem practical, scheduling a C-section without medical necessity is highly discouraged. A C-section birth is certainly not “the easy way out.” This method of delivery is a serious surgery that comes with its own potential for complications.
Newborn Microbiome Colonization
There is nothing more a mother wants than for her baby to be healthy and safe as they enter this world. But what happens to a baby’s health after being delivered through the abdomen instead of the birth canal? Believe it or not, this question has everything to do with the microbiome!
Immediately after birth, a baby experiences rapid colonization of the microbiota from his/her mother and the surrounding environment. In fact, the human microbiome is greatly influenced from the time of conception through the second year of life! Proper gut colonization and development are imperative to a newborn’s capacity to develop intestinal protection against infection and inflammatory disease.
C-section vs. Vaginal Delivery Microbiota
Research shows that the delivery method is a key determinant of the gut microbiome establishment in newborns. The largest study on this topic analyzed nearly 600 births in the United Kingdom, sampling and analyzing the DNA of microbes found in babies born vaginally and by C-section. This study found that babies born through the vaginal canal host different microbes than babies delivered by C-section. Babies born by C-section lacked the bacteria found in a healthy gut and had an abundance of opportunistic bacteria commonly associated with hospitals. As for the vaginally delivered babies, commensal (healthy) bacteria made up most of their gut population.
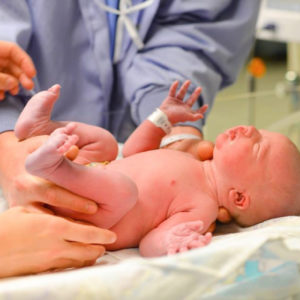
Why do these microbial differences occur?
Firstly, one reason for these microbial differences involves the ingestion of the maternal vaginal microbiota. Babies delivered by C-section do not come in contact with this microbiome, which is a critical step in an infant’s colonization process. Secondly, the differences in microbiota likely has to do with antibiotic use. Because a C-section is a serious surgical procedure, mothers receive antibiotics to prevent any harmful infections that could occur with surgery. These antibiotics can cross the placenta, directly impacting the baby’s microbiome.
Ways to Manage Baby’s Microbiome After C-section
While all of this information may seem very doom and gloom for the microbiome of a C-section baby, don’t fret! There are solutions!
Breastfeeding After C-section
One of the most important things a mother can do after having a C-section is to breastfeed her newborn. Maternal breast milk can actually promote the colonization and maturation of the baby’s gut microbiome! Breast milk is dominated by several genera of microbiota. Specifically, Bifidobacterium and Lactobacillus spp. have been demonstrated in cultures to transfer to the newborn gut.

Prebiotics & Breast Milk
Maternal breast milk also contains important prebiotics. These prebiotics are called human milk oligosaccharides (HMOs), which are sugar molecules that promote the growth of specific beneficial microbial communities, including Bifidobacterium spp. Bifidobacteria are important for preventing the growth of pathogenic organisms and for promoting immunological and inflammatory responses. Studies have shown C-sections to possibly be associated with increased risks of childhood asthma and allergic rhinitis. However, breastfeeding in early infancy has been shown to help lessen these risks compared to those who did not breastfeed after a C-section birth.
Quality Probiotic Supplementation
Although maternal breast milk is the ideal source of nutrition for newborns whenever possible, sometimes delays and other complications occur when trying to breastfeed. But even if breastfeeding is an issue, research has demonstrated that the consumption of infant formula with added high-quality probiotics promoted the development of a newborn gut microbiome similar to that of breastfed infants! Probiotics have also been shown to help the mother’s microbiome. As mentioned earlier, mothers often receive a course of antibiotics when having a C-section, which alters the composition of the mother’s microbiome as well as the baby’s microbiome. Remember, it is always recommended to speak with your healthcare provider before incorporating any new product into your supplement routine.
Vaginal Seeding
You may have heard of another possible solution for aiding the microbiome of C-section babies called “vaginal seeding.” This means taking a swab from the new mother’s vaginal microbiome and placing it into the mouth, nose, and skin of the baby following a C-section delivery. The concept behind this practice is that the vaginal swab will help establish the infant’s microbiome, similar to a baby born vaginally. Although this approach makes sense logically, it’s still considered experimental and is not routinely recommended. If a mother wishes to perform vaginal seeding, it is important to have a thorough discussion with their obstetric provider to acknowledge the potential risk of transferring pathogenic organisms and the ways to mitigate that risk through testing.
Conclusion
A mother’s mind, body, and soul are the pathway into this world for every human being on this planet. Talk about a magnificent accomplishment! As we’ve discussed, there are so many complexities to giving birth, and learning how to navigate everything is undoubtedly overwhelming. Thank you to all the strong and resilient mothers on this planet. We wouldn’t be here without you!

The content in this post is not intended to be professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health providers with any questions you may have regarding a medical condition.
Written by Kelsy Armstrong, Entegro Health
Sources:
- Allan Walker, M.D. “Supporting Your Newborn’s Health: Intestinal Colonization After Elective Cesarean Section.” Harvard Health Blog. July 2019, https://www.health.harvard.edu/blog/supporting-your-newborns-health-intestinal-colonization-after-elective-cesarean-section-2019070517262.
- American College of Obstetricians and Gynecologists. “Vaginal Seeding.” ACOG Clinical. Nov. 2017, https://www.acog.org/clinical/clinical-guidance/committee-opinion/articles/2017/11/vaginal-seeding.
- Barile D, Rastall R.A. “Human Milk and Related Oligosaccharides as Prebiotics.” Curr Opin Biotechnol. 2013;24:214–219.
- Bode L. “Human Milk Oligosaccharides: Prebiotics and Beyond.” Nutr Rev. 2009;67(Suppl. 2):S183–S191.
- Callaway E. “C-section Babies are Missing Key Microbes.” Nature. Sept. 2019, https://www.nature.com/articles/d41586-019-02807-x.
- Center for Disease Control and Prevention. “Births.” National Center for Health Statistics. Feb. 2022, https://www.cdc.gov/nchs/fastats/delivery.htm.
- “Cesarean Section- A Brief History.” U.S. National Library of Medicine, Part 1. July 2013, https://www.nlm.nih.gov/exhibition/cesarean/part1.html.
- Chu D. M., et al. “Maturation of the Infant Microbiome Community Structure and Function Across Multiple Body Sites and in Relation to Mode of Delivery.” Nat. Med. 2017;23, 314–326.
- Chu S., Zhang, Y., Jiang, Y., et al. “Cesarean Section Without Medical Indication and Risks of Childhood Allergic Disorder, Attenuated by Breastfeeding.” Sci Rep. 2017;7, 9762. https://doi.org/10.1038/s41598-017-10206-3.
- Coppa G.V., et al. “The First Prebiotics in Humans: Human Milk Oligosaccharides.” J. Clin. Gastroenterol. 2004;38:S80–S83.
- Dominguez-Bello, M.G., et al. “Partial Restoration of the Microbiota of Cesarean-Born Infants Via Vaginal Microbial Transfer.” Nature Medicine. 2016; 22.3: 250-253.
- Guaraldi F., Salvatori G. “Effect of Breast and Formula Feeding on Gut Microbiota Shaping in Newborns.” Front Cell Infect. Microbiol. 2012;2:94.
- Kim G., Bae J., Kim M. J., Kwon H., Park G., Kim S. J., Choe Y. H., Kim J., Park S. H., Choe B. H., Shin H., Kang B. “Delayed Establishment of Gut Microbiota in Infants Delivered by Cesarean Section.” Frontiers in Microbiology. 2020;11, 2099. https://doi.org/10.3389/fmicb.2020.02099.
- Lozupone C. A., Stombaugh J. I., Gordon J. I., Jansson J. K., Knight R. “Diversity, Stability and Resilience of the Human Gut Microbiota.” Nature. 2012;489 220–230.
- Mayo Clinic Staff. “Mayo Clinic, C-section.” June 2020, https://www.mayoclinic.org/tests-procedures/c-section/about/pac-20393655.
- Mueller N. T., et al. “The Infant Microbiome Development: Mom Matters.” Trends in Molecular Medicine. 2015;21,2:109-17. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4464665/.
- Shao Y., Forster S.C., Tsaliki E., et al. “Stunted Microbiota and Opportunistic Pathogen Colonization in Caesarean-Section Birth.” Nature. 2019;574, 117–121. https://doi.org/10.1038/s41586-019-1560-1.
- Sudo N., et al. “The Requirement of Intestinal Bacterial Flora for the Development of an IgE Production System Fully Susceptible to Oral Tolerance Induction.” J. Immunol. 1997;159:1739–1745.
- Wampach L., et al. “Birth Mode is Associated with Earliest Strain-Conferred Gut Microbiome Functions and Immunostimulatory Potential.” Nat. Commun. 2018; 9, 5091.
- World Health Organization. “Caesarean Section Rates Continue to Rise, Amid Growing Inequalities in Access.” World Health Organization News. June 2021, https://www.who.int/news/item/16-06-2021-caesarean-section-rates-continue-to-rise-amid-growing-inequalities-in-access.


 New customers! Get 11% OFF your first Flourish order with Code FRESHSTART11
New customers! Get 11% OFF your first Flourish order with Code FRESHSTART11