Lyme Disease
Lyme Disease x Gut Health
Lyme Disease is caused by the corkscrew-shaped bacterium Borrelia burgdorferi. The bacterium is introduced to a human host through the bite of an infected tick, most often deer ticks. These little critters are common in the Northeast and Midwest. However, Lyme Disease can be found throughout the US.

The disease itself is often called the great imitator because many of the symptoms present similarly to other diseases like chronic fatigue or fibromyalgia. The bacteria mount a systemic attack with a wide variety of individual responses. Often the infecting bite is caused by an adolescent tick, also called a nymph. These little guys are tiny so the human host may not even be aware a bite even happened.
The Most Common Signs and Symptoms
Early (3 – 30 days post-bite)
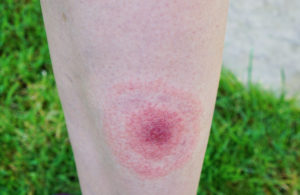
- Bullseye rash – A rash with a red center surrounded by a circle of clear skin, enclosed in a red circle; often warm to the touch but rarely itchy
- Fever, chills, headache, fatigue, muscle and joint aches, swollen lymph nodes may be present instead of a rash
Delayed (days to months after bite)
- Severe headaches and neck stiffness caused by inflammation in the brain and spinal cord
- Facial palsy – drooping on one or both sides of the face
- Severe joint pain and swelling, often in the knees or other large joints
- Pain in tendons, muscles, joints, and bones that comes and goes
- Irregular heartbeat – often feels like a flutter
- Nerve pain
- Shooting pains, numbness, or tingling in hands or feet
- Severe abdominal pain, changes in GI motility

So, what is Lyme Disease and what does it have to do with gut health?
As previously mentioned, the pathogenic bacteria Borrelia burgdorferi are spiral-shaped. In microbiology, a spiral-shaped bacterium is called a spirochete. These spirochete bacteria are very effective at survival because they can bury and hide themselves in intra and extracellular tissues, shielding them from the body’s first general attack. Cue the general tiredness, fever, and achiness. After they survive the first round of attack, the body sends a second overreacting phase that leaves chronic inflammation.
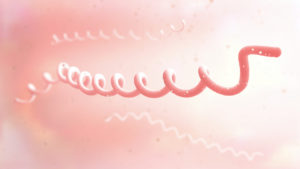
Chronic inflammation following infection is not well understood. Because inflammation and the immune system work so closely together, it makes sense to take a look at the condition of the gut. If the human host was not treated with antibiotics or was treated late, the Borrelia burgdorferi may not have been killed off. If not treated early, the host may still suffer from chronic inflammation.
Getting the gut right may play a role in helping the body overcome
Although the manifestations of Lyme Disease on the heart, brain, and joints are well studied, some research points to damage to the gut as well. Some researchers even suggest a ‘Bell’s Palsy of the gut.” Meaning a temporary paralysis of the gut. One of the biggest challenges of Lyme Disease is how differently the disease manifests in each individual. Is this due to the length of time the tick is attached to the body? Is it dependent on the general/immune/gut health of the individual prior to infection? Could there be a genetic connection? 
The connection between gut health and disease is still in the early stages of understanding. As technology and our understanding of the entire gut microbiome progresses, perhaps we will better understand the disease process of Lyme Disease.
The content in this post is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health providers with any questions you may have regarding a medical condition.
Sources
https://www.lymedisease.org/lyme-outsmarts-immune-system/
https://www.cdc.gov/lyme/index.html
https://www.lymebasics.org/reference-information/gastrointestinal-complications-of-lyme-disease/
https://www.lymebasics.org/wp-content/uploads/2019/02/GI02-BELLS-PALSY-of-the-GUT-Sherr.pdf
Schefte, D. F., & Nordentoft, T. (2015). Intestinal Pseudoobstruction Caused by Chronic Lyme Neuroborreliosis. A Case Report. Journal of neurogastroenterology and motility, 21(3), 440–442. https://doi.org/10.5056/jnm14118
Written by Lorilyn VanDyke, Entegro Health

 New customers! Get 11% OFF your first Flourish order with Code FRESHSTART11
New customers! Get 11% OFF your first Flourish order with Code FRESHSTART11